Reports
New US Guideline for Treatment of Blood Cholesterol for Prevention of Atherosclerotic Cardiovascular Disease
This report is based on medical evidence presented at sanctioned medical congress, from peer reviewed literature or opinion provided by a qualified healthcare practitioner. The consumption of the information contained within this report is intended for qualified Canadian healthcare practitioners only.
MEDICAL FRONTIERS - American Heart Association (AHA) Scientific Sessions 2013
Dallas, Texas / November 16-20, 2013
Dallas - The first public presentation of the latest American College of Cardiology (ACC)/American Heart Association (AHA) practice guidelines took place during a special plenary session at the AHA Scientific Sessions 2013. The new guideline for the treatment of blood cholesterol to prevent atherosclerotic cardiovascular disease (ASCVD), which has generated widespread comment since its release, represents a change from previous guidelines. Based on clinical evidence, the focus of treatment has shifted from treating LDL-cholesterol targets to prevention of events in four groups of primary or secondary prevention patients considered most likely to benefit from statin therapy. Non-statin therapies, alone or combined with statins, are not recommended as first-line treatment.
Chief Medical Editor: Dr.Léna Coïc, Montréal, Quebec
On November 12, 2013, the American College of Cardiology (ACC) and the American Heart Association (AHA), in collaboration with the National Heart, Lung, and Blood Institute (NHLBI) and other specialty societies, released 4 clinical practice guidelines focused on the assessment of cardiovascular risk, lifestyle modifications to reduce cardiovascular risk, and management of elevated blood cholesterol and body weight in adults (See 2013 ACC/AHA Practice Guidelines and Prevention Guidelines Tools, page 4). The four guidelines were among five initially commissioned by NHLBI in 2008 and turned over for development to the ACC and AHA in June 2013. A fifth guideline addressing hypertension will be initiated in early 2014. Each provides updated guidance for primary care providers, nurses, pharmacists and specialty medicine providers on how best to manage care of people at risk for cardiovascular-related diseases. The guideline recommendations are based on the highest quality evidence derived from randomized controlled trials (RCTs) and systematic reviews and meta-analyses of RCTs. Each of the guidelines was presented in Dallas on November 20 by the co-chairs of the expert panels responsible for their development.
Cholesterol Treatment
The new clinical practice guideline on the treatment of blood cholesterol in people at high atherosclerotic cardiovascular disease (ASCVD) risk (Stone NJ et al. 2013 ACC/AHA Blood Cholesterol Guideline) “represents a departure from previous guidelines because it does not focus on specific target levels of LDL-cholesterol, although the definition of optimal LDL-cholesterol has not changed,” said Dr. Neil J. Stone (Northwestern University Feinberg School of Medicine). “Instead, it focuses on defining groups in whom lowering the risk of ASCVD with appropriate intensity of statin therapy is proven to be most beneficial,” he explained. The guideline identifies four groups of patients for whom statins have the greatest chance of preventing stroke and heart attacks. These are individuals with 1) with clinical ASCVD; 2) primary elevations of LDL-C ≥190 mg/dL (4.9 mmol/L) 3) diabetes aged 40 to 75 years with LDL–C 70 to 189 mg/dL (1.7 to 4.9 mmol/L) and without clinical ASCVD, or 4) without clinical ASCVD or diabetes with LDL-C 70 to 189 mg/dL (1.7 to 4.9 mmol/L) and estimated 10-year ASCVD risk ≥7.5%. “The likely impact of the recommendations is that more people who would benefit from statins are going to be on them,” Dr. Stone predicted. The guideline authors chose to focus on the use of statins after a detailed review of other cholesterol-lowering drugs. “Statins were chosen because their use has resulted in the greatest benefit and the lowest rates of safety issues. No other cholesterol-lowering drugs are as effective as statins,” said Dr. Stone. It is important to monitor response and adherence in patients on statin therapy, he noted. “Focus on adherence and don’t add other therapies indiscriminately,” he advised. However, there is a role for other cholesterol-lowering drugs in patients who have an inadequate response to a statin or who are statin-intolerant, he added.
Secondary Prevention
In patients with ASCVD aged ≤75 years, the guideline recommends high-intensity statin therapy, i.e., daily doses that have been shown to lower LDL-cholesterol by ≥50%. On the basis of evidence from RCTs, these are atorvastatin 40-80 mg or rosuvastatin 20-40 mg (Table 1).
Table 1.
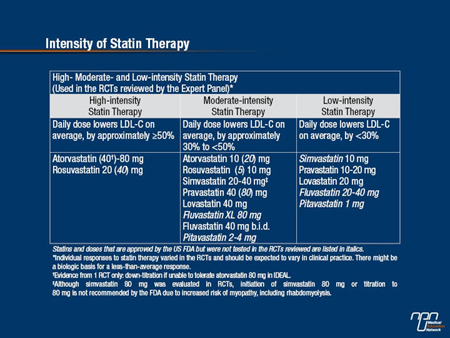
“In patients aged over 75 years, initiating moderate-intensity statin seems to make the best sense in terms of efficacy and safety,” Dr. Stone noted. A moderate-intensity statin daily dose lowers LDL-cholesterol by 30% to <50% (Table 1). Moderate-intensity statin doses may be preferred especially in patients with a history of hemorrhagic stroke or those of Asian ancestry.
Primary Prevention
“Before initiating statin therapy for primary prevention, clinicians and patients must engage in a discussion of the potential for ASCVD risk reduction benefits, potential for adverse effects, drug-drug interactions, and patient preferences,” Dr. Stone stressed. “We believe that personalized medicine is the way to go; we want to put the patient back in the equation,” he declared. Individuals with LDL-cholesterol ≥190 mg/Dl (4.9 mmol/L) should receive high-intensity statin therapy or the maximally tolerated dose. Individuals with diabetes and a 10-year ASCVD risk of ≥7.5% should receive high-intensity statins and <7.5%, moderate-intensity statin therapy. “Not everyone with a ≥7.5% 10-year ASCVD risk will be given statin therapy. Everybody considered for primary prevention has first to go through the patient-physician risk discussion,” Dr. Stone stressed. “The risk discussion will be crucial in older age groups,” he added. “I want to emphasize we are not recommending statins for over 75s for primary prevention. Although there is good evidence in secondary prevention, at least in the early years after age 75, primary prevention area is a research gap, so we don’t have data,” he said.
Risk Assessment
To estimate the 10-year risk for an ASCVD event, the guideline recommends the new Pooled Cohort ASCVD Risk Equations developed by an expert panel co-chaired by Dr. Donald M. Lloyd-Jones (Northwestern University Feinberg School of Medicine, Chicago) (Goff DC Jr. et al. 2013 ACC/AHA Cardiovascular Risk Guideline). The equations have been broadened to include assessment for risk for stroke as well as myocardial infarction. “We were leaving a lot of risk on the table by focusing on coronary heart disease alone,” Dr. Lloyd-Jones said. “But by including stroke in our new algorithm we can better calculate overall cardiovascular risk, especially in women and African-Americans.” The algorithm is also more relevant to low- and middle-income countries, where a large proportion of cardiovascular events are strokes, observed Dr. George A. Mensah (NHLBI).
The new equations were derived from data sets from NHLBI-sponsored cohort studies such as the Atherosclerosis Risk in Communities Study (ARIC), the Cardiovascular Health Study, and the Coronary Artery Risk Development in Young Adults (CARDIA) study, as well as the Framingham Original and Offspring studies. The variables included in the risk assessment are sex, age, race, total cholesterol, HDL-cholesterol, systolic blood pressure, use of antihypertensive therapy, diabetes, and smoking status (Table 2). “These [equations] also allow us to be selective and smart about whom we identify as being at high enough risk for cardiovascular disease that it would merit starting drug therapy to help prevent it. And we know that the higher someone’s risk, the more likely that person is to benefit from being on a medication,” Dr. Lloyd-Jones said. The new equations can be used to assess 10-year ASCVD risk in non-Hispanic White and African-American men and women aged 40-79 years old. The guideline also provides methods to determine lifetime risk of coronary heart disease and stroke in younger adults. “At present there are insufficient data to do robust risk estimates for Hispanic, East Asian, and South Asian Americans, but we look forward to being able to include those portions of the population in future,” Dr. Lloyd-Jones added.
Table 2.
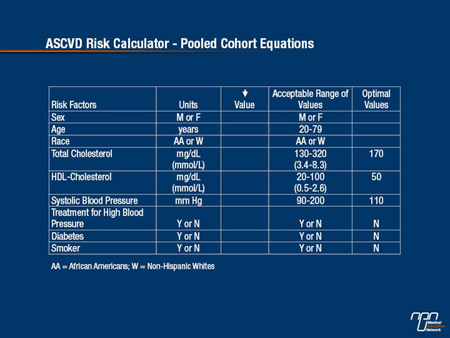
Evidence did not support using newer risk markers, but 4 markers emerged as potentially helpful where uncertainty remains after risk calculation: family history of premature CVD; high sensitivity C-reactive protein (hsCRP) ≥2 mg/dL; coronary artery calcium (CAC) score ≥300 Agatston units, and ankle brachial index (ABI) <0.9. Carotid intima-media thickness (CIMT) is not recommended for routine measurement in clinical practice for risk assessment for a first ASCVD event. “This new algorithm gives us much better information about understanding where our patient is in the risk spectrum, so that we can start the conversation, Dr. Lloyd-Jones said. However, he acknowledged that more work may be needed to improve the guidelines. When compared with non-Hispanic Whites, the estimated 10-year risk for ASCVD is generally lower in Hispanic-American and Asian-American populations and higher in American-Indian populations. “Hence, the lack of ethnic-specific risk algorithms are an important gap in our efforts to understand and prevent ASCVD in these populations,” the guideline authors stated. Answering criticism that the algorithm may overestimate ASCVD risk by as much as 75-150% (Ridker P, Cook N. Lancet Published online Nov 19, 2013), Dr. Lloyd-Jones pointed out that the criticism was based on calculations made in populations that were healthier than the broad US population. “I'm not at all surprised that our equations, which are representative of the broad US population, would over-predict in groups like those,” he pointed out.
Lifestyle as Foundation
Dr. Stone stressed the importance of adherence to a heart-healthy lifestyle. Lifestyle modifications for ASCVD risk reduction, both before and in concert with the use of statin therapy are included in the new guideline on lifestyle management to reduce cardiovascular risk (Eckel RH et al. 2013 AHA/ACC Lifestyle Management Guideline). The recommendations include adhering to a heart-healthy diet, regular exercise habits, avoidance of tobacco products, and maintenance of a healthy weight. “The cornerstone of all guidelines dealing with cholesterol is a healthy lifestyle,” said Dr. Stone. “That is particularly important in the young, because preventing high cholesterol later in life is the first and best thing someone can do to remain heart-healthy. On the other hand, if someone already has atherosclerosis, lifestyle changes alone are not likely to be enough to
prevent heart attack, stroke, and death, and statin therapy will be necessary.” Dr. Stone also emphasized the importance of the new obesity guidelines for cardiovascular risk reduction (Jensen MD et al. 2013 AHA/ACC/TOS Obesity Guideline).
Future Needs
To fill gaps in current evidence in cholesterol treatment, future RCTs will be needed to determine the optimal age at which to initiate statin therapy to reduce ASCVD risk, as well as to determine the optimum duration of statin therapy, Dr. Stone noted. Statin therapy for primary prevention should be evaluated in adults aged >75 years. Non-statin therapies should be compared with submaximal statin doses to determine whether they reduce ASCVD risk in statin-intolerant patients. Outcome in RCTs of new lipid-modifying agents, to determine whether they incrementally reduce ASCVD events when added to evidence-based statin therapy are needed. “There is a lot more to do in risk assessment,” Dr. Lloyd-Jones observed, “particularly short- and long-term ASCVD risk assessment and outcomes in all race/ethnic groups, across the age spectrum, and in women and men.”