Reports
The Canadian Malnutrition Task Force: Guiding Strategies to Reduce In-hospital Malnutrition Morbidity
This report is based on medical evidence presented at sanctioned medical congress, from peer reviewed literature or opinion provided by a qualified healthcare practitioner. The consumption of the information contained within this report is intended for qualified Canadian healthcare practitioners only.
RESOURCE LINE - Nutrition
December 2011
Guest Editors: Heather Keller, RD, PhD, FDC
Co-chair, Canadian Malnutrition Task Force Professor, Department of Family Relations and Applied Nutrition, University of Guelph , Toronto, Ontario
Johane P. Allard, MD, FRCPC
Co-chair, Canadian Malnutrition Task Force, Professor, Departments of Medicine and Nutritional Sciences, Director, Division of Gastroenterology, University of Toronto, Guelph, Ontario
The Canadian Malnutrition Task Force: Guiding Strategies to
Reduce In-hospital Malnutrition Morbidity
Despite evidence that malnutrition is common in hospitalized patients and a risk factor for adverse outcomes, few institutions have implemented systematic programs for screening and treatment. In response to data that associate malnutrition in hospitalized patients with increased morbidity and mortality, the Canadian Malnutrition Task Force (CMTF) is working to define strategies that will increase awareness of the impact of malnutrition and to identify the components of an effective diagnosis and treatment methodology. A preliminary survey and report completed in 2011 generated evidence that the prevalence of malnutrition in Canadian hospitals is high and that nutrition assessment independent of clear clinical signs of malnutrition is poor. Data from a larger, ongoing survey are expected to further encourage a more aggressive approach to assessment at admission in order to more readily and uniformly identify malnutrition even when clinical signs are not immediately evident.
Malnutrition is common among hospitalized patients. The precise prevalence depends on definition, but the yield for screening at admission when identifying both those who are malnourished and those at risk of malnutrition is substantial. In a 2011 Canadian Malnutrition Task Force (CMTF) survey of Canadian hospitals, 33% to 45% of the patients evaluated upon admission were at risk or malnourished according to several methods of nutrition assessment. The presence of malnutrition predicted an adverse outcome, including a higher risk of inhospital mortality.
These results were not unexpected based on a sizeable literature from studies of hospitalized patients previously conducted in Canada and in other countries such as The Netherlands and Sweden.1,2,3 In Singapore, where a cohort study also found malnutrition in approximately onethird of patients, it was a significant predictor of mortality (HR 4.4; P<0.001), was associated with a 2.3-day increase
in hospital stay (P<0.001) and predicted higher costs.4 These types of data have periodically inspired a variety of initiatives to address and defuse malnutrition as an adverse risk factor in hospitalized patients. The reasons that relatively few hospitals have adopted such initiatives are likely driven, at least in part, by confusion about how to best define malnutrition as well as uncertainty about how to develop programs that will incorporate a systematic and cost-effective approach for preventing and treating malnutrition within routine patient care.
Data generated by the preliminary and ongoing survey of Canadian hospitals are being used by the CMTF to develop strategies to tackle these issues. While most comprehensive care facilities employ dietitians to intervene when malnutrition is readily evident, a more proactive approach appears to be justified for occult levels of nutrition insufficiency. Overall, the available data, including those derived from the preliminary survey, suggest malnutrition can be an insidious process that is commonly overlooked in the absence of significant and visible weight loss. Use of aggressive diagnostic and treatment strategies is supported by the evidence, including CMTF data, that
malnutrition generates preventable morbidity and mortality. Screening is appropriate because of the high prevalence of malnutrition and the relative advantages of reversing nutritional deficiencies in their earliest stage.
CMTF Cohort Study: Preliminary Results
Nine hospitals participated in the preliminary prospective cohort study conducted by the CMTF. The data presented in 2011 at the European Society of Parenteral and Enteral Nutrition (ESPEN) evaluated 160 patients treated at 3 hospitals. The far larger ongoing study now includes 11 hospitals, but this may be further expanded. All patients at these centres are undergoing a nutrition assessment at admission and discharge. Outcome data are collected 30 days’ post-discharge.
At the admission screening, the broad array of measures or analyses carried out in both the preliminary and ongoing studies included or includes Subjective Global Assessment (SGA), measures of plasma albumin and C-reactive protein (CRP), anthropometry and a validated tool for identifying malnutrition called the Nutritional Risk Screening assessment (NRS 2002). A CMTF-designed screening tool consisting of determining whether there had been recent weight loss, reduced food intake for longer than 1 week and a low body mass index (BMI) is also being employed. The objectives of this study are to assess the prevalence of malnutrition in hospitalized patients in Canada; to evaluate the change in nutritional status over the course of the hospitalization; and to evaluate whether malnutrition extends length of hospital stay or adversely affects outcomes, including 30-day mortality and readmission rates.
In the preliminary analysis, 33% of patients had an NRS 2002 score of 3 or greater, which indicates malnutrition, at admission. SGA rankings of B and C, which correspond to moderate and severe risk of malnutrition, were given to 35.6% and 9.4% of patients, respectively. The average CRP level at admission was 30.2 mg/L. The CMTF-designed screening tool indicated that more than half of patients were at risk for malnutrition. As expected, the Charlson co-morbidity index was significantly higher in patients with an SGA grade of C relative to those with a grade of A (well nourished) or B. Patients given an SGA grade of C also had a lower BMI.
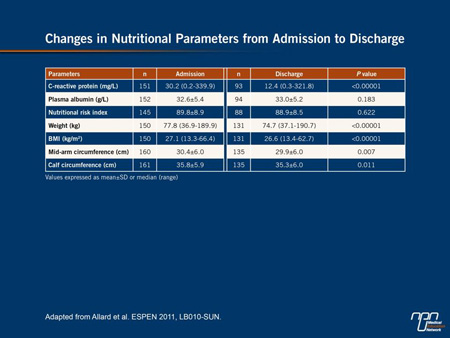
Over the course of hospitalization, plasma albumin levels were relatively unchanged and CRP levels declined dramatically (from 30.2 to 12.4 mg/L; P=0.00001), but nutritional parameters deteriorated, including weight (from 77.8 to 74.7 kg; P<0.00001), mid-arm circumference (from 30.4 to 29.9 cm; P=0.007) and calf circumference (from 35.8 to 35.3 cm; P=0.011) (Table 1).
Table 1.
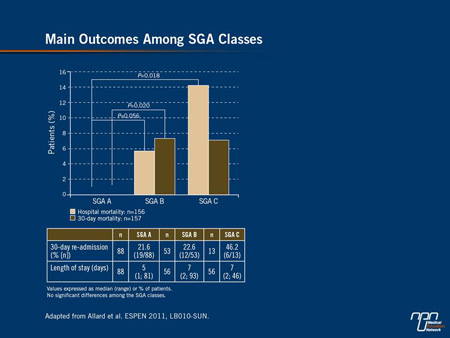
When outcomes were compared, those given an SGA grade of B or C had higher in-hospital mortality than those with SGA grade A. Patients with SGA grade B also had a higher 30-day mortality than those with grade A (Figure 1). There was no other significant difference in outcomes.
Figure 1.
CMTF Mandate: Guiding Hospitals to Screening
The final results of the CMTF Cohort Study are expected to further document a high prevalence of malnutrition and generate greater detail about how malnutrition correlates with adverse outcomes among patients admitted to acute care hospitals in Canada. As similar conclusions have already been drawn by previously published studies, the more important role of the final data will be to generate information about what strategies may be appropriate to routinely identify patients who either are malnourished or are at high risk of malnutrition on admission. In addition, the CMTF will attempt to use the data to guide strategies that will reduce the barriers to identification and treatment of malnutrition.
Of these barriers, lack of familiarity with the principles of malnutrition screening and management among health care workers may be among the most significant. Based on a survey conducted at hospitals participating in the CMTF study, physicians acknowledged this limitation. In the survey, 316 physicians responded to a 48-item questionnaire designed to elicit a self-assessment about relative understanding of malnutrition, interest in the treatment of malnutrition and perception of the relevance of malnutrition to patient care. The
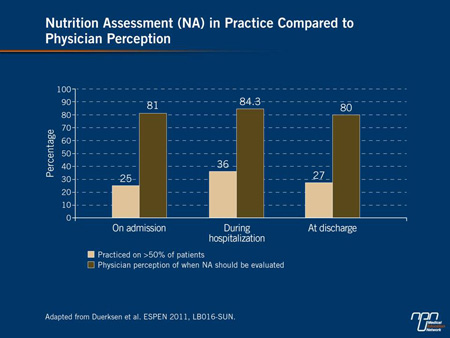
survey revealed an important disconnect between appreciation of the potential importance of malnutrition and current practice. Specifically, 80% to 84% of the responding physicians acknowledged that nutrition assessment should be conducted upon admission, during hospitalization and at discharge, but only about one-quarter to one-third acknowledged that such an assessment occurred in most patients (Figure 2).
Figure 2.
The survey results also indicated that institutional support for malnutrition screening is limited. Although tube feeding protocols were available to 63% of physicians and a nutrition support team was available to 55%, protocols for identifying malnutrition were only available to 37.9%. Even fewer reported that education on nutrition assessment was provided to medical staff at their institution. Yet 90% of the
physicians reported that they would like greater access to tools for diagnosing and managing malnutrition, and 80% specifically reported that greater access to dietitian consults would be helpful.
Developing guidelines for malnutrition screening is not a straightforward enterprise for many reasons. The first is that clinically significant malnutrition in the hospitalized patient is not well defined. From a practical perspective, detailed nutrition evaluations on every hospitalized patient may not always be appropriate or well accepted. From data generated by the ongoing cohort study, the goal will be to
identify simple measures of nutrition insufficiency that are best applied for risk stratification. When integrated into routine intake protocols, such methodology could be used primarily to identify levels of risk, including those who require a nutrition consult.
Based on the survey, which generated results comparable to a similar study conducted in Scandinavia,5 a lack of comfort among health care personnel with their own level of knowledge regarding nutrition screening has exacerbated the effect of an absence of standardized guidelines. Although the physician survey also found a reluctance to expend time on nutrition screening, those without expertise in this area may overemphasize the requirements of simple screening tools. The preliminary results of the CMTF survey indicate that screening for nutritional status may be performed quickly with available tools and little specific training. Patients with evidence of malnutrition can then be referred for a more advanced level of care.
The relative willingness within an institution to create a reproducible, self-sustaining protocol is another significant obstacle to malnutrition screening. Moreover, the CMTF survey indicated that even those institutions that encourage nutritional screening may fail to designate a chain of responsibility to ensure that screening is performed consistently. Although it is reasonable to assume that those responsible for case management will either assess nutritional status or designate someone for this task, the frequency with which malnutrition goes undiagnosed indicates that more formal structures are needed.
System-wide strategies, such as requiring screening values to be included in the medical record, have the potential to greatly improve compliance. In addition, detection of malnutrition or a high risk of malnutrition should trigger processes that will ensure that the problem is addressed. For those at low to moderate risk, this may be limited only to periodic monitoring, whereas more substantial strategies, including referral to the nutrition support staff, should be initiated when risk is moderate to high. Optimal programs will include quality control to review outcomes and confirm delivery of best practices.
Based on the data collected by the CMTF so far, the path to wide dissemination of effective nutrition screening programs throughout Canada will require several steps. The first is to ensure broad support for nutrition screening programs by providing data that demonstrate their benefits. Hospital administrators, for example, may not readily recognize the need for specific nutrition screening programs in an institution that has developed a nutrition support staff. While the screening that identifies malnutrition at an early stage may reduce hospital stay to provide its own cost justification, the most important impetus for screening is the opportunity to improve outcomes.
The next step will be to encourage the development of reproducible methodology for screening and treatment that is suited to the current institutional protocols. In the absence of evidence-based guidelines for selecting an algorithm, it is hoped that the general principles and relative benefits of available screening tools identified by the CMTF will provide guidance to institutions selecting programs that can be effectively integrated into existing patient care structures.
Early detection of patients at risk for or at an early stage of malnutrition provides an opportunity to avoid the more complex and costly interventions required as nutrition deficiencies reach an advanced stage. This may simply involve encouraging and monitoring food consumption. At a more advanced stage, oral nutritional supplements (ONS) can be offered either to supplement or replace meals, providing the balance of proteins and nutrients that may be less reliably provided by diet alone. By encouraging oral intake of nutrients, the expense of parenteral nutrition can be avoided.
Importantly, the most sophisticated of the current formulations of ONS are effective at restoring the protein loss that often defines malnutrition in patients with acute disease. However, other characteristics may be important. For example, products that add short-chain fructo-oligosaccharides to nourish resident gut bacteria may play an important role in restoring the ability of the gastrointestinal tract to properly absorb nutrients. While many ONS may be effective in a given individual, it is useful to recognize that these are not interchangeable.
The overall goals of the ongoing efforts by the CMTF are to shift the culture regarding the diagnosis and treatment of malnutrition in the hospital setting. Practice has been slow to adapt despite the large body of evidence associating malnutrition with adverse outcomes. While the most effective programs will be those that are adapted to fit with current practice methods at a given institution, it is hoped that the CMTF initiatives can refocus attention to the problem, encourage education and training and guide institutions in integrating screening and treatment programs into standard hospital practice.
Summary
The evidence that malnutrition is a source of adverse outcomes in hospitalized patients is plentiful but has not sufficiently altered practice in Canadian hospitals. The CMTF has embarked on a multifaceted study to draw attention to the problem of malnutrition and the potential strategies for screening and early intervention. The goal is to foster protocols for evaluating nutritional status at the time of admission, periodically over the course of the hospital stay and upon discharge. Simple screening tools have the potential to improve patient care.
References
1. Singh et al. Nutrition 2006;22:350-4.
2. Kruizenga et al. Clin Nutr 2003;22:147-52.
3. Westergren et al. J Nutr 2009;8:20-4.
4. Lim et al. Clin Nutr 2011; Epub ahead of print.
5. Mowe et al. Clin Nutr 2008;27:196-202.