Reports
St. Michael’s Hospital
This report is based on medical evidence presented at sanctioned medical congress, from peer reviewed literature or opinion provided by a qualified healthcare practitioner. The consumption of the information contained within this report is intended for qualified Canadian healthcare practitioners only.
PHYSICIAN PERSPECTIVE - Get with the PROTOCOL - A Regional Perspective on the Evidence and Resulting Changes in ACS Protocol
April 2013
Reviewed and edited by:
David H. Fitchett, MB, ChB, MD, FESC, FRCPC
Cardiologist
St. Michael’s Hospital
Toronto, Ontario
Introduction
Antiplatelet therapy in the management of acute coronary syndromes (ACS) has recently been revised at St. Michael’s Hospital. The altered algorithm is designed to provide significant reductions in risk of major cardiovascular (CV) events by employing newer antiplatelet agents compared to the previous standard of clopidogrel and ASA. Guided by the large clinical trials that underlie the revised algorithm, the specific recommendations allow for the clinical gains from greater antiplatelet effect, including in some cases, a lower risk of death. They also balance benefit with an acceptably low risk of major or minor bleeding. Due to the fundamental importance of deactivating platelets to alter the natural history of evolving ACS events, optimal use of antiplatelet therapy should be considered an essential strategy for improving the prognosis of ACS. The protocol is consistent with the 2012 CCS Antiplatelet Guidelines.
Previous Standard: Need for Improvement
The dual antiplatelet strategy of clopidogrel and ASA in patients presenting with ACS has been a widely employed standard for more than 10 years. However, rates of CV events in ACS populations remain substantial. In the landmark CURE study, 10% of those receiving clopidogrel plus ASA went on to a recurrent myocardial infarction (MI), a persistent arterial occlusion or died of a CV cause despite the 20% reduction with the combination relative to ASA alone.1 This study was performed in patients with non-ST elevation MI (NSTEMI). In the CLARITY-TIMI 28 trial, conducted in patients with ST elevation MI (STEMI), the residual risk of death, stroke or MI was 9% in the group receiving clopidogrel plus ASA despite a 31% reduction in risk of a major CV event relative to ASA alone.2
Since those studies established this dual antiplatelet combination as a standard in ACS, two large ACS trials have proven that more effective antiplatelet therapy will further reduce CV risk. The PLATO study tested ticagrelor initiated early after presentation in both NSTE ACS and STEMI patients.3 The TRITON-TIMI 38 study studied prasugrel in ACS patients scheduled for a percutaneous coronary intervention (PCI).4 Data from these trials provide an opportunity to improve outcomes over the previous clopidogrel plus aspirin standard.
In the TRITON-TIMI 38 study, 13,608 ACS patients were randomized. Antiplatelet therapy was not administered until the coronary anatomy had been shown to be suitable for PCI. In the experimental arm, patients received a loading dose of prasugrel (60 mg) followed by maintenance prasugrel (10 mg daily). The comparator arm received a loading dose of clopidogrel (300 mg) followed by maintenance clopidogrel (75 mg daily). Both groups received ASA. Approximately 25% of the ACS events were STEMI and the remaining NSTEMI.
Relative to clopidogrel, prasugrel reduced the risk of the composite end point of death from CV cause, MI or stroke by 19% (HR 0.81; P<0.001). The risk of major bleeding on prasugrel was increased by 32% (HR 1.32; P=0.03) relative to clopidogrel. There was no difference in mortality. The authors concluded that the greater protection against ischemic events must be weighed against an increased risk of bleeding, but post-hoc analyses provided guidance for candidate selection.
Figure 1.
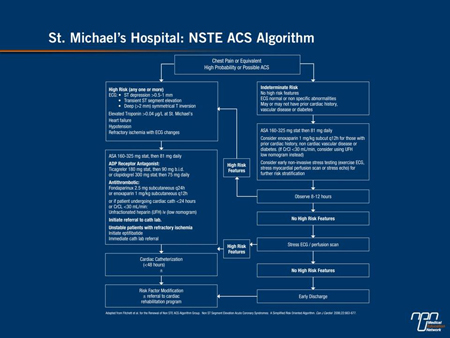
In the PLATO trial, individuals admitted to hospital with ACS were randomized regardless of planned procedure or pre-hospital antiplatelet treatment. The experimental arm received a loading dose of ticagrelor (180 mg) followed by maintenance ticagrelor (90 mg twice daily). The comparator arm received a loading dose of clopidogrel (300 or 600 mg) followed by maintenance clopidogrel (75 mg daily). Both groups received ASA. Approximately 37% of the 18,624 patients randomized had STEMI and the remaining had NSTEMI.
Relative to clopidogrel, ticagrelor reduced the risk of the composite end point of death from vascular causes, MI or stroke by 16% (HR 0.84; P<0.001). The difference in total major bleeding (11.6% vs. 11.2%; P=0.43) did not reach statistical significance but non-CABG major bleeding was significantly increased (4.5% vs. 3.8%; P=0.026). Noteworthy to antiplatelet trials, ticagrelor was associated with a 22% reduction (HR 0.78; nominal P<0.001) in all-cause mortality.
New Data Translated into Clinical Practice
The revised treatment algorithms for antiplatelet therapy in ACS patients are designed to improve outcome based on the recent trials. While all ACS patients should be initiated on ASA immediately, the second antiplatelet agent is defined by the diagnosis, the planned strategies for intervention and specific patient characteristics. Several large organizations have altered ACS antiplatelet guidelines on the basis of the PLATO and TRITON-TIMI 38 trials, but algorithms at the regional or hospital level are appropriate because of differences in ACS care.
Figure 2.
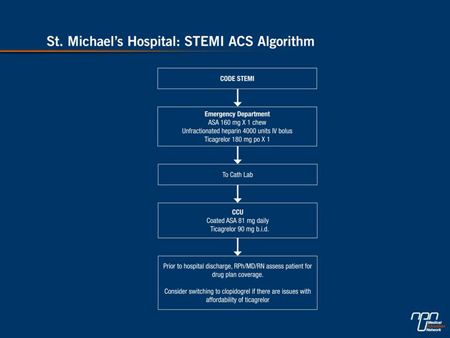
At regional centres, including St. Michael’s Hospital, the data generated by the trials can be applied directly. Although prasugrel and ticagrelor both improve outcomes in ACS patients, St Michael’s Hospital chose to use ticagrelor for all ACS because it was more applicable to a wider range of ACS patients treated in the tertiary care centre than prasugrel. Furthermore it was felt desirable to avoid the complexities of having three anti-platelet agents available.
In ACS patients at St. Michaels Hospital, ticagrelor is now the preferred medication for dual antiplatelet strategy with ASA. It is started at first medical contact or in higher risk patients even if they have received a loading dose of clopidogrel. Clopidogrel is used in patients on an oral anticoagulant or who are at a high risk of bleeding, especially intracranial.
Relevance of New Algorithm to Regional Centres
The new antiplatelet therapies improve the outcome in ACS patients. However indications and limitations for the individual agents differ, such that the choice of the optimal agent should be tailored for the patient and the institution. All centres should develop treatment algorithms that are adjusted for these factors. The algorithm at St. Michael’s Hospital may or may not be relevant to nearby community centres.
There are compelling data to conclude that implementation of more modern strategies for appropriate candidates will improve ACS outcomes including a reduction in mortality. The implementation and adherence to treatment guidelines in the management of ACS has been associated with statistically significant improvements in outcome. In an observational analysis that included 350 academic and non-academic centers, a stepwise 10% reduction in in-hospital mortality rates was associated with each 10% increase in adherence to evidence-based guidelines.5
Conclusion
The first-line antiplatelet strategies in ACS patients have been revised. The newer agents ticagrelor and prasugrel provide an important opportunity to improve outcome relative to clopidogrel when any of these agents is combined with ASA. In ACS patients, the advantage of ticagrelor over clopidogrel in appropriately selected patients includes a mortality reduction. The guidelines developed by St. Michael’s Hospital were designed specifically to identify these opportunities in a readily applied algorithm.
Questions & Answers
Q: What is your perspective on the benefit-to-risk ratio that the newer antiplatelet agents offer within the revised algorithm for reducing the risk of thrombosis within an acceptable rate of bleeding?
A: Ticagrelor compared to clopidogrel in ACS improved the primary outcome of CV death/MI/stroke by 16%. The number needed to treat to prevent one thrombotic event was 52. The number needed to treat to harm with a major bleed was 143. Thus there is an acceptable benefit to risk ratio, especially when mortality is reduced 22%.
Q: The studies that led to changes in the guidelines compared therapies in different populations. What insights can you offer on why it was important to prove superiority of prasugrel or ticagrelor over clopidogrel in different ACS groups (STEMI and NSTE ACS)?
A: The management of STEMI and NSTE ACS is quite different, with immediate reperfusion having benefit in STEMI but not in NSTE ACS. Consequently it is important to determine that the new agents are superior to the previous standard clopidogrel in all scenarios.
Q: What is your point of view on the possible side effects associated with the newer agents vs. the opportunity to improve outcomes?
A: The major side effect of the new agents compared to clopidogrel is the increased bleeding rates. For prasugrel increased bleeding rates limit its use in patients who have had prior stroke or TIA. Off target effects of ticagrelor such as dyspnea and sinus arrest do not appear to have major effects in clinical trials, however may become more problematic in real world applications.
Q: The algorithm introduces some decision points not previously required when all patients were treated with clopidogrel plus ASA. What action needs to be taken to improve outcomes?
References
1. Yusuf et al. Effects of clopidogrel in addition to aspirin in patients with acute coronary syndromes without ST-segment elevation.
N Engl J Med 2001;345(7):494-502.
2. Sabatine et al. Addition of clopidogrel to aspirin and fibrinolytic therapy for myocardial infarction with ST-segment elevation. N Engl J Med 2005;352(12):1179-89.
3. Wallentin et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N Engl J Med 2009;361(11):1045-57.
4. Wiviott et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N Engl J Med 2007;357(20):2001-15.
5. Peterson et al. Association between hospital process performance and outcomes among patients with acute coronary syndromes. JAMA 2006;295(16):1912-20.